Plantar fasciitis is one of the most common causes of heel pain. Whereby the plantar fascia, a thick band of tissue that runs across the bottom of the foot, and connects the heel bone to the toes, becomes inflamed. The plantar fascia plays an important role in the normal biomechanics of the foot. Providing support for the arch and acting as a shock absorber.
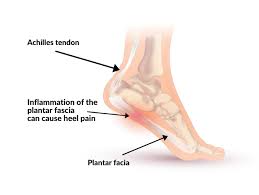
Plantar fasciitis is often an overuse injury that can be due to repetitive strain causing micro-tears in the fascia. Repeated stretching and tearing of the fascia can irritate or inflame it, but can also occur as a result of trauma.
Even though plantar fasciitis can develop without an obvious cause, some factors can increase your risk of developing this condition. They include:
Before you consider what course of action to take, educating yourself of this condition is key. You need to know that the symptoms may take weeks or even months to improve. Following advice given from a Doctor or therapist, for example. Resting from aggravating activities initially, icing and stretching will help in the acute phase, reducing pain and symptoms. You should also be aware of the importance of a home exercise plan, along with any other treatments you may be having.
Treatments that your therapist may look to use can include, but are not limited to; sports massage/soft tissue manipulation, stretch and refer strengthening exercises of the musculature of the lower limb, such as the calves and plantar fascia, joint mobilisations/manipulations and the use of taping to reduce pain symptoms. A combination of these techniques is said to be more effective than just one or the other.
Self-care/ at home exercises:
These are some exercises that you could expect your therapist to refer to you after having treatment to help manage the symptoms of plantar fasciitis:
Alex Broadhead (May 2022)